Abstract
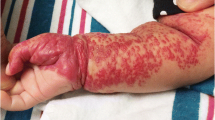
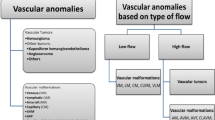
Most haemangiomas and vascular malformations are identified according to clinical criteria. A good knowledge of the classification and clinical characteristics of the vascular anomalies is necessary when managing these patients. However, some cases are challenging either because of an atypical presentation (e.g., soft-tissue mass with normal overlying skin) or because of classification difficulties. Doppler US and MRI are the two main imaging modalities that allow classification of the vascular anomalies and are useful in those clinically uncertain cases to establish the correct diagnosis. This aids the choice of the most appropriate treatment and to inform the parents of the prognosis. High-resolution grey-scale and Doppler US allow excellent visualization of most superficial masses. Doppler US is the easiest way to assess the haemodynamics of a vascular lesion and to clarify a doubtful diagnosis between a haemangioma and vascular malformation. MRI is the best technique for evaluating the extent of the lesions and their relationship to adjacent structures. While newly developed drugs from angiogenesis research labs are awaited, radiologists have an important role in the treatment of haemangiomas and vascular malformations. Intervention remains crucial in cases of alarming haemangiomas and venous malformations (VM), lymphatic malformations (LM) and arteriovenous malformations (AVM). A multidisciplinary team, including paediatricians, haematologists, surgeons and radiologists, must manage the problem cases both in terms of diagnostic work-up and therapeutic options. This paper will briefly discuss the imaging findings and treatment of vascular anomalies.












Similar content being viewed by others
References
Mulliken JB, Glowacki J (1982) Classification of pediatric vascular lesions. Plast Reconstr Surg 70:120–121
Mulliken JB, Fishman SJ, Burrows PE (2000) Vascular anomalies. Curr Probl Surg 37:517–584
Dubois J, Patriquin HB, Garel L et al (1998) Soft-tissue hemangiomas in infants and children: diagnosis using Doppler sonography. AJR 171:247–252
Konez O, Burrows PE (2002) Magnetic resonance of vascular anomalies. Magn Reson Imaging Clin N Am 10:363–388
Metry DW, Hawrot A, Altman C et al (2004) Association of solitary, segmental hemangiomas of the skin with visceral hemangiomatosis. Arch Dermatol 140:591–596
Metry DW, Dowd CF, Barkovich AJ et al (2001) The many faces of PHACE syndrome. J Pediatr 139:117–123
Léauté-Labrèze C, Taïeb A (2008) Efficacy of beta-blockers in infantile capillary haemangiomas: the physiopathological significance and therapeutic consequences. Ann Dermatol Venereol 135:860–862
Boon LM, Enjolras O, Mulliken JB (1996) Congenital hemangioma: evidence of accelerated involution. J Pediatr 128:329–335
North PE, Waner M, James CA et al (2001) Congenital nonprogressive hemangioma: a distinct clinicopathologic entity unlike infantile hemangioma. Arch Dermatol 137:1607–1620
Dubois J, Garel L, David M et al (2002) Vascular soft-tissue tumors in infancy: distinguishing features on Doppler sonography. AJR 178:1541–1545
Robertson RL, Robson CD, Barnes PD et al (1999) Head and neck vascular anomalies of childhood. Neuroimaging Clin N Am 9:115–132
Trop I, Dubois J, Guibaud L et al (1999) Soft-tissue venous malformations in pediatric and young adult patients: diagnosis with Doppler US. Radiology 212:841–845
Paltiel HJ, Burrows PE, Kozakewich HP et al (2000) Soft-tissue vascular anomalies: utility of US for diagnosis. Radiology 214:747–754
Siegel MJ (2001) Magnetic resonance imaging of musculoskeletal soft tissue masses. Radiol Clin North Am 39:701–720
Li W, David V, Kaplan R et al (1998) Three-dimensional low dose gadolinium-enhanced peripheral MR venography. J Magn Reson Imaging 8:630–633
Dubois J, Garel L, Abela A et al (1997) Lymphangiomas in children: percutaneous sclerotherapy with an alcoholic solution of zein. Radiology 204:651–654
Molitch HI, Unger EC, Witte CL et al (1995) Percutaneous sclerotherapy of lymphangiomas. Radiology 194:343–347
Ogita S, Tsuto T, Nakamura K et al (1994) OK-432 therapy in 64 patients with lymphangioma. J Pediatr Surg 29:784–785
Baskin D, Tander B, Bankaoğlu M (2005) Local bleomycin injection in the treatment of lymphangioma. Eur J Pediatr Surg 15:383–386
Muir T, Kirsten M, Fourie P et al (2004) Intralesional bleomycin injection (IBI) treatment for haemangiomas and congenital vascular malformations. Pediatr Surg Int 19:766–773
Orford J, Barker A, Thonell S et al (1995) Bleomycin therapy for cystic hygroma. J Pediatr Surg 30:1282–1287
Zhong PQ, Zhi FX, Li R et al (1998) Long-term results of intratumorous bleomycin-A5 injection for head and neck lymphangioma. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 86:139–144
Zulfiqar MA, Zaleha AM, Zakaria Z et al (1999) The treatment of neck lymphangioma with intralesional injection of bleomycin. Med J Malaysia 54:478–481
Sanlialp I, Karnak I, Tanyel FC et al (2003) Sclerotherapy for lymphangioma in children. Int J Pediatr Otorhinolaryngol 67:795–800
Sung MW, Lee DW, Kim DY et al (2001) Sclerotherapy with picibanil (OK-432) for congenital lymphatic malformation in the head and neck. Laryngoscope 111:1430–1433
Alqahtani A, Nguyen LT, Flageole H et al (1999) 25 years’ experience with lymphangiomas in children. J Pediatr Surg 34:1164–1168
Enjolras O, Riche MC, Merland JJ (1985) Facial port-wine stains and Sturge-Weber syndrome. Pediatrics 76:48–51
Jacob AG, Driscoll DJ, Shaughnessy WJ et al (1998) Klippel-Trénaunay syndrome: spectrum and management. Mayo Clin Proc 73:28–36
Gloviczki P, Driscoll DJ (2007) Klippel-Trenaunay syndrome: current management. Phlebology 22:291–298
Cohen MM Jr (2000) Klippel-Trenaunay syndrome. Am J Med Genet 93:171–175
Moodley M, Ramdial P (1993) Blue rubber bleb nevus syndrome: case report and review of the literature. Pediatrics 92:160–162
Fretzin DF, Potter B (1965) Blue rubber bleb nevus. Arch Intern Med 116:924–929
Esterly NB (1996) Cutaneous hemangiomas, vascular stains and malformations, and associated syndromes. Curr Probl Pediatr 26:3–39
Wiedemann HR, Burgio GR (1986) Encephalocraniocutaneous lipomatosis and Proteus syndrome. Am J Med Genet 25:403–404
Clark RD, Donnai D, Rogers J et al (1987) Proteus syndrome: an expanded phenotype. Am J Med Genet 27:99–117
Samlaska CP, Levin SW, James WD et al (1989) Proteus syndrome. Arch Dermatol 125:1109–1114
Darmstadt GL, Lane AT (1994) Proteus syndrome. Pediatr Dermatol 11:222–226
Garzon MC, Huang JT, Enjolras O et al (2007) Vascular malformations. Part II: associated syndromes. J Am Acad Dermatol 56:541–564
Hovius SE, Borg DH, Paans PR et al (1996) The diagnostic value of magnetic resonance imaging in combination with angiography in patients with vascular malformations: a prospective study. Ann Plast Surg 37:278–285
Taschner CA, Gieseke J, Le Thuc V et al (2008) Intracranial arteriovenous malformation: time-resolved contrast-enhanced MR angiography with combination of parallel imaging, keyhole acquisition, and k-space sampling techniques at 1.5 T. Radiology 246:871–879
Reinacher PC, Stracke P, Reinges MH et al (2007) Contrast-enhanced time-resolved 3-D MRA: applications in neurosurgery and interventional neuroradiology. Neuroradiology 49:S3–S13
Saleh RS, Lohan DG, Villablanca JP et al (2008) Assessment of craniospinal arteriovenous malformations at 3 T with highly temporally and highly spatially resolved contrast-enhanced MR angiography. AJNR 29:1024–1031
Wu Y, Kim N, Korosec FR et al (2007) 3D time-resolved contrast-enhanced cerebrovascular MR angiography with subsecond frame update times using radial k-space trajectories and highly constrained projection reconstruction. AJNR 28:2001–2004
Ziyeh S, Strecker R, Berlis A et al (2005) Dynamic 3D MR angiography of intra- and extracranial vascular malformations at 3 T: a technical note. AJNR 26:630–634
Enjolras O (1997) Classification and management of the various superficial vascular anomalies: hemangiomas and vascular malformations. J Dermatol 24:701–710
Guttmacher AE, Marchuk DA, White RI Jr (1995) Hereditary hemorrhagic telangiectasia. N Engl J Med 333:918–924
Jessen RT, Thompson S, Smith EB (1977) Cobb syndrome. Arch Dermatol 113:1587–1590
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dubois, J., Alison, M. Vascular anomalies: what a radiologist needs to know. Pediatr Radiol 40, 895–905 (2010). https://doi.org/10.1007/s00247-010-1621-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-010-1621-y